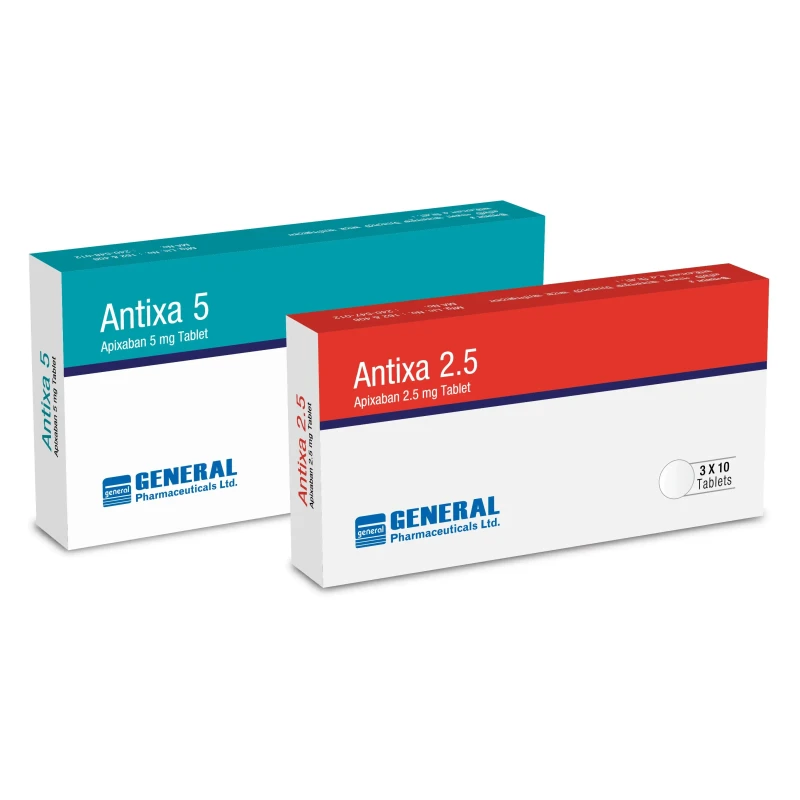

Antixa Tablet, Apixaban 5 mg
Inhouse product
-
৳11.40
৳12.00 -
৳42.75
৳45.00 -
৳16.63
৳17.50 -
৳2.14
৳2.25 -
৳9.50
৳10.00
Reviews & Ratings
Indications
Antixa is a factor Xa
inhibitor indicated:
- To reduce the risk of stroke
and systemic embolism in patients with nonvalvular atrial fibrillation
- For the prophylaxis of deep
vein thrombosis (DVT), which may lead to pulmonary embolism (PE), in
patients who have undergone hip or knee replacement surgery
- For the treatment of DVT and
PE, and for the reduction in the risk of recurrent DVT and PE following
initial therapy
* রেজিস্টার্ড চিকিৎসকের পরামর্শ মোতাবেক ঔষধ সেবন করুন'
Pharmacology
Apixaban acts by
inhibiting coagulation, and thus prevents development of blood clots. As a
result of FXa inhibition, apixaban prolongs clotting tests such as prothrombin
time (PT), INR, and activated partial thromboplastin time (aPTT). Changes
observed in these clotting tests at the expected therapeutic dose, however, are
small, subject to a high degree of variability, and not useful in monitoring
the anticoagulation effect of apixaban.
Dosage &
Administration
Recommended Dose: The recommended dose of Apixaban for most
patients is 5 mg taken orally twice daily.
Dosage Adjustments: The recommended dose of Apixaban is 2.5 mg
twice daily in patients with any 2 of the following characteristics: age ≥80
years, body weight ≤60 kg, serum creatinine ≥1.5mg/dl.
CYP3A4 and P-gp
inhibitors: When Apixaban is
coadministered with drugs that are strong dual inhibitors of cytochrome P450
3A4 (CYP3A4) and P-glycoprotein (P-gp) (e.g. ketoconazole, itraconazole,
ritonavir, clarithromycin) the recommended dose is 2.5 mg twice daily.
Missed Dose: If a dose of Apixaban is not taken at the
scheduled time, the dose should be taken as soon as possible on the same day
and twice-daily administration should be resumed. The dose should not be
doubled to make up for a missed dose.
Discontinuation for
Surgery and Other Interventions: Apixaban should be discontinued at least 48 hours prior to
elective surgery or invasive procedures with a moderate or high risk of
unacceptable or clinically significant bleeding. Apixaban should be
discontinued at least 24 hours prior to elective surgery or invasive procedures
with a low risk of bleeding or where the bleeding would be non-critical in
location and easily controlled.
Switching from or to
Apixaban: Switching from
warfarin to Apixaban: Warfarin should be discontinued and Apixaban started when
the international normalized ratio (INR) is below 2.0.
Switching from
Apixaban to warfarin: Apixaban affects
INR, so that INR measurements during co-administration with warfarin may not be
useful for determining the appropriate dose of warfarin. If continuous
anticoagulation is necessary, discontinue Apixaban and begin both a parenteral
anticoagulant and warfarin at the time the next dose of Apixaban would have
been taken, discontinuing the parenteral anticoagulant when INR reaches an
acceptable range.
Switching between
Apixaban and anticoagulants other than warfarin: Discontinue one being taken and begin the
other at the next scheduled dose.
* রেজিস্টার্ড চিকিৎসকের পরামর্শ মোতাবেক ঔষধ সেবন করুন'
Interaction
Antixa is a substrate
of both CYP3A4 and P-gp. Inhibitors of CYP3A4 and P-gp increase exposure to
Antixa and increase the risk of bleeding. Inducers of CYP3A4 and P-gp decrease
exposure to Antixa and increase the risk of stroke.
Contraindications
Apixaban is
contraindicated in patients with the following conditions: Active pathological
bleeding. Severe hypersensitivity reaction to Apixaban (i.e. anaphylactic
reactions).
Side Effects
Antixa can cause a
skin rash or severe allergic reaction.
Pregnancy &
Lactation
Pregnancy: There are no adequate and well-controlled
studies of Apixaban in pregnant women. Treatment is likely to increase the risk
of hemorrhage during pregnancy and delivery. Apixaban should be used during
pregnancy only if the potential benefit outweighs the potential risk to the
mother and fetus.
Labor and Delivery: Safety and effectiveness of Apixaban during
labor and delivery have not been studied in clinical trials. Consider the risks
of bleeding and of stroke in using Apixaban in this condition.
Nursing Mothers: It is unknown whether Apixaban or its metabolites
are excreted in human milk. Women should be instructed either to discontinue
breastfeeding or to discontinue Apixaban therapy, taking into account the
importance of the drug to the mother.
Precautions &
Warnings
Increased Risk of
Stroke with Discontinuation of Antixa Discontinuing Antixa in the absence of
adequate alternative anticoagulation increases the risk of thrombotic events.
An increased rate of stroke was observed during the transition from Antixa to
warfarin in clinical trials in patients with nonvalvular atrial fibrillation.
If Antixa must be discontinued for a reason other than pathological bleeding,
consider coverage with another anticoagulant.
Use in Special
Populations
Hepatic Impairment: No dose adjustment is required in patients
with mild hepatic impairment. Because patients with moderate hepatic impairment
may have intrinsic coagulation abnormalities and there is limited clinical
experience with Antixa in these patients, dosing recommendations cannot be
provided Antixa is not recommended in patients with severe hepatic impairment
Renal Impairment: The dosing adjustment for moderate renal
impairment is described above. No data inform use in patients with creatinine
clearance <15 ml/min or on dialysis.
Pediatric Use: Safety and effectiveness in pediatric
patients have not been established.
Geriatric Use: Of the total subjects in clinical studies of
Antixa, >69% were 65 and older, and >31% were 75 and older. The effects
of Antixa on the risk of stroke and major bleeding compared to warfarin were
maintained in geriatric subjects.
Overdose Effects
There is no antidote
to Antixa. Overdose of Antixa increases the risk of bleeding. Activated
charcoal may be useful in the management of Antixa overdose.
Therapeutic Class
Anti-coagulants,
Anti-platelet drugs, Fibrinolytics (Thrombolytics), Oral Anti-coagulants
Storage Conditions
Keep in a dry place
and store below 30°C. Protect from light and keep out of the reach of children.
Frequently Bought Products
Nebita Tablet, Nebivolol Hydrochloride 2.5 mg
Bost Tablet, Vitamin B1, B6 & B12 100 mg+200 mg+200 mcg
Myocard Tablet, Bisoprolol Fumarate 2.5 mg
Briva Oral Solution 50 ml bottle, Brivaracetam 50 mg/5 ml
Cipro-A Tablet, Ciprofloxacin 500 mg
Product Queries (0)
Login Or Registerto submit your questions to seller
Other Questions
No none asked to seller yet
-
৳11.40
৳12.00 -
৳42.75
৳45.00 -
৳16.63
৳17.50 -
৳2.14
৳2.25 -
৳9.50
৳10.00










![ORSaline Fruity Oral Powder (20's pack), Oral rehydration salt [flavore & glucose based] 13.47 gm/sachet](https://www.old.skpharma.com.bd/public/uploads/all/OfFxNvZ722eXFPiorfasJm6o9hR5XrgRlIREkCWC.jpg)





